
ON THIS PAGE: You will find out more about,

Our body systems are replete with various cells that control the effective functioning of every part of us. The efficient interactions of these cells in the body impact our growth, maintenance and well-being. Cancer occurs when these cells are no longer in charge of the specific functions they perform or when they totally lose control of their own growth.
This uncontrolled growth of abnormal cells that divide rapidly often results in infiltration and destruction of tissue, thereby bringing the normal control mechanism of the body to a halt.
This experience is usually common in adults than in children because what causes cancer in children is quite different from what causes cancer in adults. For instance, unlike most adult cancers, childhood cancers are scarcely linked to lifestyle or environmental factors, and mostly associated with genetics and heredity.
According to the U.S National Cancer Institute, the annual Cancer diagnosis for children is about 10,000 while adults account for 1.5 million cases.
In this article, more attention will be placed on childhood cancers, shedding more light on the most common pediatric cancers.
Cancer patients between the ages of 0-14 years are usually diagnosed with the following cancers:
Leukaemia is the cancer of the blood and the bone marrow. This term originates from the Greek words, leukos, meaning white, and haima, meaning blood. Leukaemia is cancer that affects the white blood cells by multiplying its underdeveloped abnormal cells in high numbers.
The white blood cells, also called leukocytes, are responsible for fighting infections and destroying foreign bodies and diseases that threaten the health. Since the white blood cells are in charge of fighting pathogens, the harmful manipulations of these cells results in a suppression of the immune system, making the body open to frequent infections.
Like most cancers, the cause of leukaemia is not known but can be traced to environmental or hereditary factors like family history. Also, children with Down syndrome are more susceptible to leukaemia.
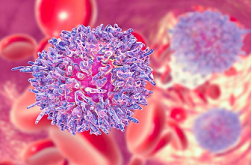
According to the American Society of Clinical Oncology (ASCO), the most common symptoms of leukaemia in children include,
The most common types of leukaemia in children are:
Acute myeloid leukaemia (AML): a condition in which excess immature white blood cells are developed, hindering the growth of normal blood cells. It affects children between the ages of 2-8.
Acute lymphoblastic leukaemia (ALL): a condition which spikes the production of many lymphoblasts, thus creating less room for healthy blood cells. It affects children between the ages of 2-5.
Treatment for Leukaemia range from chemotherapy to radiation therapy, and in some cases, bone marrow transplant.
Thanks to the advancement in health-technology, medical research and clinical trials, a considerable number of children treated for leukaemia get cured of the disease.
Known as the second most common type of cancer in children, brain cancers account for 15% of pediatric cancers (ACCO).
As the name implies, Brain cancers are the growth of abnormal cells that affect the brain tissues. The brain is one of the most sensitive parts of the human makeup, which makes pediatric brain cancers very challenging to treat.
Since the brain is the command centre of the central nervous system, it is essential to detect brain tumours early. Most of these tumours are difficult to operate or outright inoperable because of their location (especially as the skull which encompasses the brain has little or no space for the tumours).
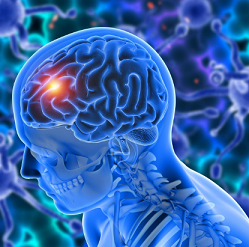
Brain tumours are either malignant or benign. Malignant brain tumours contain cancerous cells, while the benign tumours do not.
Common symptoms of brain cancers in children are very tricky to determine because they are usually similar to other common childhood ailments.
Symptoms include:
There are several types of brain cancers, but the most common is Gliomas. This is the umbrella term for all brain tumours that originate in glial cells of the brain. According to the American Cancer Society, about half of all brain and spinal cord tumours in children are Gliomas.
The Columbia University Department of Neurology lists some of these tumours to include:
Other brain tumours that are not Gliomas include:
Treatment for pediatric brain tumours is dependent on factors such as the child’s age, the location of the tumour and the stage of cancer. Some of the treatment options for such cancers are neurosurgery, chemotherapy, radiotherapy, proton beam therapy, and steroids.
Lymphoma is a broad term that encompasses the cancers of the lymphatic system. This type of childhood cancer makes the blood cells develop rapidly, split up, and live longer than normal. It affects the lymphatic system, which is responsible for transporting lymph which protects the body against diseases. Lymph carry antibodies which fight infections in the body.
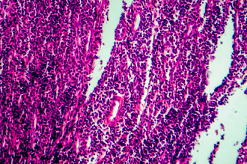
Symptoms of Lymphoma in children include,
The two major types of lymphomas are:
Lymphoma also affects children from 0-14 years, although Hodgkin lymphoma rarely affects children less than 5 years of age. Both Hodgkin and non-Hodgkin lymphomas are more common in male children than female.
The causes of Lymphoma are not known, but viral infections like the Human Immune Virus (HIV) and Epstein-Barr virus (EBV) increase the risk factors for being diagnosed with Lymphoma. Other factors include any activity that weakens the immune system like previous chemotherapy or the intake of immunosuppressive drugs.
Treatment for Lymphoma depends on the particular type that is being treated. But most of the treatments include chemotherapy, radiotherapy and in some cases, surgery.
According to a recent study, children have more chances of beating cancers than adults as survival rates for children with cancer is much higher than that of their adult counterparts.
This is not to go without saying that children who beat cancer will have to be extra careful in their habits and lifestyle for the rest of their adult lives as survivors. For obvious reasons, the long term side effects of after-cancer treatment impact the quality of life of childhood cancer survivors later in life.

Indeed, it can be devastating to handle a kid with cancer. First, learning that one’s child has cancer comes with its fair share of shock and down feelings.
But it is noteworthy that children respond better to cancer treatments. This is to say that your kid has a higher chance of surviving.
For the child, this period is equally very crucial. It is not uncommon for the diagnosed child to have to stay away from school or give up playtime with other kids. The child’s new reality may now include frequent visits to the hospital, taking lots of medications, tests and therapy.
As a parent, it will be helpful to explain to the kid what is happening in very simple terms, while reassuring him/her that the phase is only temporary. This is so as to avoid the feelings of anxiety and fear overwhelming the child.
You can also encourage the child to keep a journal to write down their feelings, a canvas to paint, lively music to listen to, and lots of inspiring storybooks to read.
The whole experience of cancer diagnosis and treatment can be daunting for both the child and the parents. Try your best not to always show gloominess around the child. Find ways outside your child’s presence to express your sadness or vent your anger. Just don’t do those around the child patient as all they need is hope and assurance.
Again, your child’s diet is of utmost importance in this period. Ensure that the child is on a balanced diet, especially one that goes well with his/her treatment plan.
You can read more on Nutritional Needs for Kids with Cancer.
Know that you do not have to do this alone. If need be, get the support of a pediatric psychotherapist or counsellor to talk to your child once in a while.
You can find helpful information on other types of Cancer in the links below:
What You Need to Know About Cancer
Medical Disclaimer: KompleteCare™ aims to improve the quality of life for everyone with fact-based content about the nature of diseases, preventive care, behavioral health conditions, treatment options and their related outcomes. We publish material that is researched, cited, edited and reviewed by licensed medical professionals. The information we provide is not intended to be a substitute for professional medical advice, diagnosis or treatment. It should not be used in place of the advice of your physician or other qualified healthcare provider.
healthcareSeptember 1, 2020
ParentingSeptember 2, 2020
healthcareAugust 20, 2025
healthcareSeptember 10, 2025
NutritionSeptember 16, 2025








Parbriz Iveco Daily 6 Box Body 2014
My programmer is trying to convince me to move to
.net from PHP. I have always disliked the
idea because of the costs. But he’s tryiong none the less.
I’ve been using Movable-type on a number of websites for about a year and am worried about
switching to another platform. I have heard fantastic
things about blogengine.net. Is there a way I can import all my wordpress content into it?
Any kind of help would be really appreciated! https://vanzari-parbrize.ro/parbrize/parbrize-iveco.html
Parbrize kia k2500
hello!,I love your writing very a lot! percentage
we communicate more about your article on AOL? I require a specialist on this house to unravel my problem.
Maybe that’s you! Looking forward to see you. https://vanzari-parbrize.ro/index.php?cauta=parbriz+kia
Ukachukwu George Onyewuezi
Thanks my pretty medical personnel, infact this is very educative , informative ,medicative more importantly global awakening nd awareness thanks for a very wonderful nd painstaking research ❤
Ernest Ibifiri
A very insightful article. Please keep up the good work.
Harmony
You are too good with the explanation,this is really an informative and educative writeup. Thanks so much, you are just good babe.
Faith
It’s quite educative as always.
Austine Edung
Wow!!! What an edifying and insightful piece. It’s a wake up call for parents and the society at large. Thanks to our scientitists and researchers who bury valuable hours into seeking a cure for this scourge on humanity called cancer. I foresee a breakthrough in the very near future.
Thanks for this beautiful write-up!
Ginika Oluchi Okeke
We share in your optiminism Mr Austine.
A breakthrough is surely in sight.
Flourish
This is very precise and educative
Oche OGOLEKWU
The issue of “health” by any means should be prioritized among other human collections. If human body does the work, it should be replicated appropriate healthy “environments” . The “environment” here means acquaintance with useful health platforms like this (K)KOMPLETECARE ONLINE PLATFORM.
Health discourses of this platform are always time related especially in critical periods of global pandemic and other health issues as contained script above.
In fact, this platform is a weaponry forum to discover and being schooled with knowledge as well as substantive approaches to apply in times like this.
God bless the initiator of this platform.
Ginika Oluchi Okeke
Thanks. Truer words have never been spoken
IFECHUKWU
Very informative. I look forward to reading more write-ups
Akoja Faith
This is a lovely write-up. Health is indeed wealth. Thanks for the eye opening on the subject of cancer. This would go a long way in curbing the incessant cases of this dreaded disease. Thanks so much for this insightful piece Ginika.
Nwaru Rita
Very Apt and wonderful, weldone dear
Chiamaka Cynthia
Exactly the reason I keep coming back for more. This article is educative and tends to sensitize the society at large
Franklin Udosen
Very inspiring especially with my background of working in a cancer centre… In my experience the love and support from family might be the main catalyst for a patients quest for survival in beating cancer.. In healthy environment is as good as a good chemotherapy in my opinion.. Keep up the good work, Gini
Ruth
Very educative. These are common knowledge we should arm ourselves with in our day to day activities while trying to live in health. Thanks Gnika
RUTH IYEN
Very Educative I learnt alot from this I even have to read it over and over again ….Good job keep it up👍🏼👍🏼👍🏼
Anna
Kudos to you, u really detailed a vital information here concerning kids suffering from cancer , so that the society and parents whose kid are undergoing for such can no the necessary measures to handle the kids without fear, anxiety overwhelming such kid so that such child can over come the treatment
Archie
Very well detailed…
I had always thought cancer was from lifestyle and environment only.
But the write-up has shown me something novel.
Thumbs up
Gunnn Michael
Waoooo I love dis knowledge…. God bless u
Gboyega
This is a well-researched complicated topic which the author has been able to break down to allow non-medical people to comprehend easily… Thank you!
Jasmine
Very insightful read. Well researched too. I will need some excerpts for my project
Nkemjika
An eye-opening and educative piece well written.
Ajay206
Wow! Such an amazing and helpful post this is. I really really love it. It’s so good and so awesome. I am just amazed. I hope that you continue to do your work like this in the future also.